Research Article: Journal of Drug and Alcohol Research (2022) Volume 11, Issue 6
Medication Adherence of Antibiotics Used in Vulnerable Population at Selected Tertiary Care Hospital in Andhra Pradesh
Amit Kumar1*, S K Panda2, Divya S Nair3, Padala Srilakshmi3 and Sruthi Sreenivasan32Royal College of Pharmacy and Health Sciences, Berhampur, Odisha, India
3Aditya College of Pharmacy, Surampalem, Andhra Pradesh, India
Amit Kumar, Biju Patnaik University of Technology, India, Email: amitpharmacypractice@gmail.com
Received: 27-May-2022, Manuscript No. jdar-22-63492; Editor assigned: 30-May-2022, Pre QC No. jdar-22-63492 (PQ); Reviewed: 13-Jun-2022, QC No. jdar-22-63492; Revised: 20-Jun-2022, Manuscript No. jdar-22-63492 (R); Published: 27-Jun-2022, DOI: 10.4303/jdar/236182
Abstract
Aim: To determine the medication adherence towards antibiotics in vulnerable populations at selected tertiary care hospital in Andhra Pradesh.
Materials and methods: This prospective study was carried out at selected tertiary care hospital. A total of 551 vulnerable inpatients were studied for medication adherence for antibiotics prescribed. The vulnerable inpatients included in the study are pediatrics, pregnant women, geriatrics and other vulnerable patients. Socio-economic status of the patients was measured using Modified Kuppuswamy socio-economic status scale 2020 and based on this scale the patients were found to be of lower middle, upper lower and lower class. In this study the medication adherence was assessed using Morisky Medication Adherence Scale (MMAS-8). Hartwig scale was used to measure the ADRs. Socioeconomic status was correlated with medication adherence to measure the extent of association.
Results: Cephalosporins were the most commonly prescribed antibiotics in patients. The average medication adherence among the population was found to be 6.54 on the scale of 8 which suggests the adherence was medium or moderate. Geriatric patients showed the lowest adherence as compared to the other groups. A total of 56 ADRs and 57 drug interactions were reported in the study
Conclusion: Medication non-adherence is depended on the patient factors and other complications that might occur. It is also depended on the socioeconomic status of the patients. Therefore, a close counselling and monitoring is also required for inpatients. This study is on inpatients which reveals non-adherence; hence we now know what to expect on the adherence among outpatients who are rarely monitored closely.
Keywords
Antibiotics; Medication adherence; MMAS-8; Modified kuppuswamy scale 2020; Hartwig’s Scale
Introduction
Medication adherence usually refers to whether patients are taking their medication as prescribed or not. The major predictors for medication non-adherence are high pill burden, complex dosing schedule, poor knowledge of disease and treatment, chronic illness, duration of treatment, adverse effects, taking alternative medicines, socio-economic status and high cost of prescribed drugs. This medication adherence can be assessed using Morisky Medication Adherence Scale (MMAS-8) [1]. It has proved to be a valuable resource to measure the adherence using a series of questions that involves factors influencing adherence, such as forgetting to take medications or discontinuing medications without guidance. If the score is less for a patient, then they are struggling with no adherence and if a patient score higher then it shows they are more adherent to the treatment [2]. Surprisingly, non-adherence is also possible among inpatients, especially the ones where the oral administrations are taken care by the attender of the patients. This can be observed among patients who are from a socio-economically weak background. Modified Kuppuswamy socioeconomic status scale measures socioeconomic status of a person based upon education, occupation and monthly income [3]. From these scorings of medication adherence, clinicians and health organizations can identify underlying issues that prevent patients from taking their medications correctly, if at all. Total MMAS – 8 scores range from 0-8 and have been categorized into three levels of adherence; high adherence (8), medium adherence (6 to <8), low adherence (<6) [4]. Antibiotics should be consumed as prescribed by the doctors and entire course of therapy has to be completed to have complete eradication of bacterial infection. Generally, in our society patients stop taking antibiotics when they observe relief in clinical symptoms but it’s not the ideal way because the patients might be still infected and if entire course of therapy of antibiotics are not taken then this will lead to bacterial resistance or antibiotic resistance. Antibiotics controls the infection and can cause resistance of an organism against it if not properly consumed based upon prescription [5]. Antibiotic misuse can lead to unnecessary expenditure, overuse of health services, unnecessary side effects, and the possible development of antibiotic resistance [6]. Our present prospective study aims to determine the medication adherence of antibiotics in the vulnerable population (pediatric, pregnant women, elderly and the other vulnerable group in the community) who have been admitted in the hospital and prescribed with antibiotics [7]. In the current study we aimed to assess the different types of antibiotic use behavior among patients based upon adherence question mentioned in MMAS-8. Our study also determines Drug-Drug interactions and Adverse Drug Reactions (ADRs).
Materials and Methods
Our study was initiated after ethics committee clearance. The study was approved by respective Institutional Ethics Committee (IEC/IRB ref no: 650-A-EC/650-A-02/20) and all the study participants were informed about study details and informed consent was obtained. This prospective study was conducted at selected tertiary care hospital of Andhra Pradesh during the period of February 10, 2020 to December 9, 2021. Total number of patients enrolled in the study was 551. The in patients such as pediatric (<18 years), geriatric (>60 years), pregnant women (18 to 40 years) and other groups (18 to 60 years) were included in the study and socio-economic status of these patients was determined using Modified Kuppuswamy socio-economic status scale 2020 and based upon this scale the patients were found to belong to lower middle, upper lower and lower class. “Other” groups include the patients who are chronically, critically, mentally or economically compromised. Numbers of patients in each group were as follows: Pediatrics (139). Geriatrics (116), pregnant women (58) and others (238). All the above patients including male and female under antibiotics therapy were included in this study. All the out patients and patients with incomplete laboratory report were excluded. Data was collected from the patient case sheets after necessary permission was obtained from hospital authorities. Specially designed data collection form was used for data collection and Inform consent form was designed. The antibiotics prescribed were recorded in the data collection form with their dose, route, dosage form, frequency of administration, indications and duration of therapy. All the cases were subjected to check medication adherence by using Morisky Medication Adherence Scale that has 8 questionnaires (Table 1). Each “No” response was rated as “1” and each “Yes” was rated as “0” except in question 5, where each “Yes” response was rated as”1” and each “No” was rated as “0”. In question 8, for response “0”, the score was “1” and for response “4” the score was “0” whereas for responses “1, 2 and 3” the scores were “0.75, 0.5 and 0.25” respectively. We followed up the study group to check the drug interactions and this was done by using IBM Micromedex ® Web Applications Access. The interactions like antibiotic-antibiotic or antibiotic-drug (other than an antibiotic) interactions were only considered. ADRs were determined by using Hartwig Scale (based on mild, moderate and severe) [8]. Statistical analysis was done using JMP® Pro version 13.0.0 (SAS Institute Inc.).
Table 1: Morisky Medication Adherence Scale (MMAS-8).
| S.NO | MMAS-8 ADHERENCE QUESTIONS | YES | NO |
|---|---|---|---|
| 1 | Did you sometimes forget to take your medication? | 0 | 1 |
| 2 | People sometimes miss taking their medications for reasons other than forgetting, Over the past 2 weeks there any days when you did not take your medication? | 0 | 1 |
| 3 | Have you ever cut back or stopped taking your medication without telling your doctor because you felt worse when you took it? | 0 | 1 |
| 4 | When you travel or leave home, do you sometimes forget to bring your medication? | 0 | 1 |
| 5 | Did you take all your medication yesterday? | 1 | 0 |
| 6 | When you feel like your symptoms are under control, do you sometimes stop taking your medications? | 0 | 1 |
| 7 | Taking medications every day is a real inconvenience for some people. Do you ever feel hassled about sticking to your treatment plan? | 0 | 1 |
| 8 | How often do you have difficulty remembering to take all your medication? | ||
| 0. Never/Rarely | 1 | ||
| 1. Once in a while | 0.75 | ||
| 2. Sometimes | 0.5 | ||
| 3. Usually | 0.25 | ||
| 4. All the time | 0 | ||
Results
Table 2 shows that, in gender wise distribution among the total study population of 551, 282 (51.18%) were male patients and 269 (48.82%) were female patients. Two or more antibiotics were prescribed to 292 patients among the vulnerable population.
Table 2: Gender based distribution of the vulnerable group with the number of antibiotics prescribed.
| Categories | Vulnerable group | Number of antibiotics | ||
|---|---|---|---|---|
| 1 | 2 | >2 | ||
| Male (51.8%) | Other (n=142) | 56(39.44%) | 61(42.96%) | 25(17.60%) |
| Pediatric (n=68) | 37(54.41%) | 25(36.76%) | 6(8.82%) | |
| Geriatric (n=72) | 32(44.44%) | 30(41.67%) | 10(13.89%) | |
| Female (48.82%) | Other (n=96) | 45(46.88%) | 37(38.54%) | 14(14.58%) |
| Pediatric (n=71) | 31(43.66%) | 33(46.48%) | 7(9.86%) | |
| Pregnant women (n=58) | 45(77.59%) | 5(8.62%) | 8(13.79%) | |
| Geriatric (n=44) | 13(29.55%) | 21(47.73%) | 10(22.73%) | |
| Total vulnerable groups (n=551) | Other (n=238) | 101(42.44%) | 98(41.18%) | 39(16.38%) |
| Pediatric (n=139) | 68(48.92%) | 58(41.73%) | 13(9.35%) | |
| Pregnant women (n=58) | 45(77.59%) | 5(8.62%) | 8(13.79%) | |
| Geriatric (n=116) | 45(38.79%) | 51(43.97%) | 20(17.24%) | |
A total of 56 ADRs occurred during the course of the study (Table 3). Maximum ADRs occurred among geriatric patients (31) and most ADRs occurred with Cephalosporins class of antibiotics. The severity of ADRs were measured using Hartwig scale and level 1 was for ADR that required no change in treatment with suspected drug, level 2 was when ADR required the suspected drug to be held, discontinued, or changed but no antidote or other treatment was required and no increase in length of stay was there and level 3 was when ADR required the suspected drug to be held, discontinued, or otherwise changed, and/or an antidote or other treatment is required with no increase in length of stay. All the ADRs in our study were Mild (Level 1 and Level 2) and Moderate (Level 3).
Table 3: Antibiotics that caused adverse drug reactions and their severity based on Hartwig’s scale.
| Category | Antibiotics | ADRs | Hartwig Severity level | ||
|---|---|---|---|---|---|
| 1 | 2 | 3 | |||
| Pediatrics | Vancomycin (P) | Rashes (N=1) | 3 | ||
| Meropenem (P) | Clammy Skin (N=1) | 1 | |||
| Cefixime (O) | Diarrhea (N=1) | 3 | |||
| Amoxicillin, Clavulanic Acid (O) | Skin Rash (N=1) | Feeling Sick (N=2) | 3 | ||
| Mupirocin (LA) | Pain (N=1) | 3 | |||
| Sulfamethoxazole-Trimethoprim (O) | Loss Of Appetite (N=1) | 2 | |||
| Pregnant women | Amikacin (P) | Stomach Upset (N=1) | 2 | ||
| Geriatrics | Ceftriaxone (P) | Hives (N=1) | 3 | ||
| Meropenem (P) | Clammy Skin (N=1) | 1 | |||
| Sulbactam-Cefoperazone (P) | Nausea (N=5) | Vomiting (N=1) | 1 | ||
| Ceftriaxone (P) | Swelling Of Face (N=5) | Stomach Upset (N=2) | 3 | ||
| Azithromycin (O) | Abdominal Pain (N=1) | Hives (N=4) | Stomach Upset (N=1) | 3 | |
| Faropenem (O) | Diarrhea (N=1) | 3 | |||
| Cefixime(O) | Headache (N=8) | Diarrhea (N=1) | 1 | ||
| Others | Amoxycillin-Clavulanate (O) | Diarrhea (N=1) | Skin Rash (N=1) | Feeling Sick (N=1) | 3 |
| Ciprofloxacin | Abdominal Pain (N=1) | 3 | |||
| Cefotaxime (P) | Hypersensitivity (N=1) | 3 | |||
| Gentamycin (P) | Hearing Loss (N=1) | 3 | |||
| Ceftriaxone (P) | Hives (N=1) | 3 | |||
| Piperacillin-Tazobactam (P) | Bladder Pain (N=1) | Changes In Urination(N=1) | 3 | ||
| Doxycycline (O) | Severe Headache(N=1) | 3 | |||
| Cefixime (O) | Diarrhea (N=1) | 3 | |||
| Levofloxacin (O) | Constipation (N=1) | Trouble Sleeping (N=1) | 1 | ||
| Faropenem (O) | Nausea (N=2) | Vomiting (N=1) | 1 | ||
| P=Parenteral, O=Oral, LA=Local Application | |||||
Drug interactions also occurred with the prescribed antibiotics among which 89.47% where significant (moderate and serious interactions) and 22 (38.6%) serious interactions were found (Table 4). Some examples of significant interactions include interactions between levofloxacin and metformin, azithromycin and ondansetron, levofloxacin and dexamethasone, etc.
Table 4: Antibiotics that caused drug interactions and their severities.
| Vulnerable group | Severity | Drug-drug interactions |
|---|---|---|
| Pediatrics | Minor | 6 (10.53%) |
| Moderate | 0 | |
| Serious | 9(15.79%) | |
| Pregnant women | Minor | 0 |
| Moderate | 0 | |
| Serious | 0 | |
| Geriatrics | Minor | 0 |
| Moderate | 8 (14.04%) | |
| Serious | 5 (8.77%) | |
| Others | Minor | 0 |
| Moderate | 21 (36.84%) | |
| Serious | 8 (14.04%) |
One way ANOVA for medication adherence score in the study population was performed and F distribution (<0.0001) was found to be significant at 0.05 level of significance (Figure 1). A Post hoc (Tukey-Kramer test) was done at 0.05 level of significance to identify which group is significantly different. Geriatric patients appear to be far below the mean of response (6.59) indicating they had least medication adherence among all vulnerable populations.
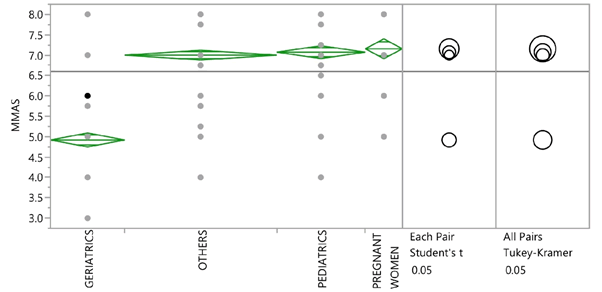
Figure 1: One way ANOVA showing MMAS score in the study population.
The scores of Morisky Medication Adherence Scale Table 5 shows least medication adherence among 98 (84.48%) geriatric patients with an average score of 4.92 on scale of 8 whereas pediatrics, pregnant women and others showed a medium adherence with an average score of 7.07 on the scale of 8. Overall average medication adherence score in the study population was found to be medium with the score of 6.54 (Tables 5 and 6).
Table 5: Medication adherence score using MMAS-8 in the study population.
| Count Row% | 3 | 4 | 5 | 5.25 | 5.75 | 6 | 6.5 | 6.75 | 7 | 7.25 | 7.75 | 8 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Geriatric (n=116) | 7 | 33 | 44 | 0 | 14 | 12 | 0 | 0 | 3 | 0 | 0 | 3 |
| 6 | 28.5 | 37.9 | 0 | 12.1 | 10.3 | 0 | 0 | 2.59 | 0 | 0 | 2.59 | |
| Others (n=238) | 0 | 5 | 18 | 2 | 1 | 13 | 0 | 5 | 124 | 0 | 1 | 69 |
| 0 | 2.1 | 7.56 | 0.8 | 0.42 | 5.46 | 0 | 2.1 | 52.1 | 0 | 0.4 | 29 | |
| Pediatrics (n=139) | 0 | 4 | 6 | 0 | 0 | 16 | 1 | 4 | 54 | 2 | 4 | 48 |
| 0 | 2.88 | 4.32 | 0 | 0 | 11.5 | 0.7 | 2.9 | 38.9 | 1.4 | 2.9 | 34.5 | |
| Pregnant women (n=58) | 0 | 0 | 1 | 0 | 0 | 9 | 0 | 0 | 28 | 0 | 0 | 20 |
| 0 | 0 | 1.72 | 0 | 0 | 15.5 | 0 | 0 | 48.3 | 0 | 0 | 34.5 |
Table 6: Average MMAS score distribution in study population based on questionnaire.
| Vulnerable groups | Q1 Average | Q2 Average | Q3 Average | Q4 Average | Q5 Average | Q6 Average | Q7 Average | Q8 Average | Score Average |
|---|---|---|---|---|---|---|---|---|---|
| Pediatrics | 1 | 0.99 | 0.99 | 0.49 | 0.99 | 0.96 | 0.95 | 0.72 | 7.07 |
| Pregnant women | 1 | 0.98 | 1 | 0.71 | 1 | 1 | 1 | 0.47 | 7.16 |
| Geriatrics | 0.54 | 0.53 | 1 | 0.08 | 0.41 | 0.97 | 0.83 | 0.56 | 4.92 |
| Others | 1 | 0.99 | 0.99 | 0.48 | 0.95 | 0.97 | 0.97 | 0.65 | 7 |
| Average | 0.89 | 0.87 | 0.99 | 0.44 | 0.84 | 0.98 | 0.94 | 0.6 | 6.54 |
The modified Kuppuswamy scale 2020 was used to know the socioeconomic status of the patients. This is done by scoring the patients based on the education, occupation and monthly income of the head of the families. According to the scale, greater the score better the socioeconomic status. This socioeconomic (SE) score was used to determine the class of the study population who were found to belong in the class of lower middle, upper lower and lower class. Chi square whole model test with goodness of fit was performed to see the correlation between socioeconomic score and MMAS score. The test showed positive slope between socioeconomic score and MMAS score which is clearly seen as inclined upward blue lines from left to right. This means that as the socioeconomic score increases, the medication adherence increases (Figure 2).
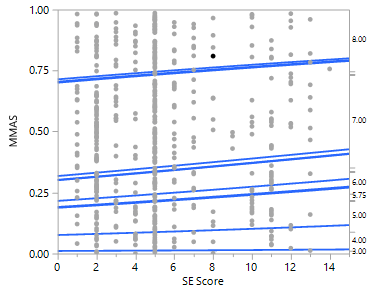
Figure 2: MMAS based on socioeconomic score (SE score).
Discussion
Incidence of ADR in our study was found to be 10.16%. Among antibiotics, Cephalosporins were mostly prescribed with most ADRs. No statistical association was found between medication adherence and drug interaction or severity of ADR. Table 6 reveals, instances like ADR and drug interactions could contribute to less medication adherence in the patients who cut back the medications without telling their doctor as they would have lost faith in the treatment thinking that it may make things worse for them (question number 3 of the MMAS-8 Scale with an average score of 0.99 and in geriatric score of 1). In the study population more than 2 antibiotics was prescribed in 292 patients. Average drugs on each prescription in the entire study population was found to be 4.15 including antibiotics. Such polypharmacy could cause inconvenience for some patients which results in unwillingness to take the medications (7th question of MMAS-8 Scale with an average score of 0.94 and for geriatrics the score is 0.83). The geriatric patients show a lower score in questions 1, 2, 4, 5 and 8 which are related in being forgetful. Poor medication adherence in geriatrics can be also due to comorbid conditions like diabetes, hypertension, thyroid disorders, arthritis, for which they are already on medications. Medication adherence also depends on the patient’s socioeconomic status of the patients. Medication non-adherence can lead to worsening of disease, increased health cost and even mortality [9]. Adherence can be improved effectively by finding out the type and cause of non-adherence and by looking into specific needs of the patient [10].
Conclusion
Adherence to medications is primary determinant for successful treatment outcomes. In the study, the level of adherence to antibiotic treatment was medium and in geriatrics it was lowest. The main reasons for medication non-adherence can be pill burden, complex dosing schedule, and comorbidity, duration of treatment, socio-economic status and high cost of prescribed branded drugs. All patients and their attenders should be educated and counseled by physicians, nurses and clinical pharmacists to adhere to the treatment plan to have better treatment outcome, prevent ADR and drug interactions. Individuals aged >60 years are on other medications due to comorbidity and the patients who have to take multiple antibiotics or antibiotics for multiple times a day are more prone to cutting back the treatment, such patients should be closely monitored and counseled to adhere to the treatment. Entire course of antibiotics should be completed by the patients in order to have complete eradication of bacteria from the body. Healthcare providers should regularly review medication regimen of the patients and should find out safe ways to reduce polypharmacy by eliminating duplicate medications and prescribe single drug which can provide same therapeutic effects as multiple drugs. In Indian context high cost of medicines plays a crucial role in medication non-adherence therefore doctors should prescribe generic drugs more which costs less than branded drugs and whenever possible should provide subsidized medicines or free medicines to patients. Doctors generally get free medicines as “physician samples” from pharmaceutical companies. Pharmaceutical companies should give emphasis on manufacturing fixed dose combination of antibiotics at affordable cost to enhance the medication adherence among the patients in the community. These steps if implemented by healthcare providers and pharmaceutical manufacturers can surely improve medication adherence among the patients. Prescribers are not to be blamed solely for the irrational or improper use of antibiotics and for less treatment outcomes in patients but patients not adhering to the prescribing guidelines are also the contributing factor for antibiotics becoming ineffective or not showing desired therapeutic response and for these effective interventions are required from healthcare providers in guiding patients so that medication non-adherence can be curtailed and quality of life of patients can be enhanced.
Acknowledgement
The authors would like to gratefully acknowledge all cooperation and support from the patients and hospital administration for facilitating this study.
Source of Funding
None.
Conflict of Interest
Nil.
References
- P.M. Ho, C.L. Bryson, J.S. Rumsfeld, Medication adherence: Its importance in cardiovascular outcomes, Circulation, 119(2009), 3028-35.
[Crossref] [Google Scholar] [PubMed] [Research Gate]
- W.Y. Lam, P. Fresco, Medication adherence measures: An overview, Biomed Res Int, (2015), 217047.
[Crossref] [Google Scholar] [PubMed] [Research Gate]
- S.M. Saleem. Modified Kuppuswamy socioeconomic scale updated for the year 2020. Ind J Foren Com Med, 7(2020).
- S. Okello, B. Nasasira, A.N.W. Muiru, A. Muyingo, Validity and reliability of a self-reported measure of antihypertensive medication adherence in Uganda. PLOS one, 11(2016).
[Crossref] [Google Scholar] [PubMed] [Research Gate]
- R.J. Fair, Y. Tor, Antibiotics and bacterial resistance in the 21st century, Perspect Medicin Chem, 6(2014), 25-64.
[Crossref] [Google Scholar] [PubMed] [Research Gate]
- V.C. Lee, The antibiotic resistance crisis: Part 1: Causes and threats, P T, 40(2015), 277-83. [Crossref]
- Vulnerable population: Who are they? Am J Manag Care, 12(13). 348-352.
[Google Scholar] [PubMed]
- G. Petrova, A. Stoimenova, M. Dimitrova, M. Kamusheva, D. Petrova, et al. Assessment of the expectancy, seriousness and severity of adverse drug reactions reported for chronic obstructive pulmonary disease therapy, SAGE Open Med, 5(2017).
[Crossref] [Google Scholar] [PubMed] [Research Gate]
- B. Jimmy, J. Jose, Patient medication adherence: Measures in daily practice. Oman Med J, 26(2011).
[Crossref] [Google Scholar] [PubMed] [Research Gate]
- J.G. Hugtenburg, L. Timmers, P.J.M. Elders, M. Vervloet, L. van Dijk, Definitions, variants, and causes of nonadherence with medication: A challenge for tailored interventions, Patient Prefer Adherence, 7(2013), 675–682.
[Crossref] [Google Scholar] [PubMed] [Research Gate]
Copyright: © 2022 Amit Kumar, et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.

