Research Article: Journal of Drug and Alcohol Research (2022) Volume 11, Issue 5
Drug Utilization Evaluation of Antibiotics used in Vulnerable Population at Selected Tertiary Care Hospital in Andhra Pradesh
Amit Kumar1*, S K Panda2, Divya S Nair3, Padala Srilakshmi3 and Sruthi Sreenivasan32Royal College of Pharmacy and Health Sciences, Berhampur, India
3Aditya College of Pharmacy, Surampalem, India
Amit Kumar, Biju Patnaik University of Technology, India, Email: amitpharmacypractice@gmail.com
Received: 02-May-2022, Manuscript No. jdar-22-63491; Editor assigned: 04-May-2022, Pre QC No. jdar-22-63491 (PQ); Reviewed: 18-May-2022, QC No. jdar-22-63491; Revised: 23-May-2022, Manuscript No. jdar-22-63491 (R); Published: 30-May-2022, DOI: 10.4303/jdar/236176
Abstract
Aim: To determine drug utilization evaluation (DUE) of antibiotics used in vulnerable populations at selected tertiary care hospital in Andhra Pradesh.
Materials and methods: This prospective study was carried out among 551 patients (vulnerable population pediatrics, pregnant women, geriatrics and other vulnerable patients) from a selected tertiary care hospital. Based on Modified Kuppuswamy socio economic status scale 2020 our study population was under lower middle, upper lower and lower class. In our study the ratio of prescribed daily dose (PDD) to WHO defined daily dose (DDD) and DOT calculation (for pediatrics) was used for drug utilization evaluation. Cost comparison study was also conducted between the prescribed branded antibiotics and their generic alternative.
Results: The study included 551 patients; males were in majority when compared to females. Cephalosporins were the most commonly prescribed antibiotics in patients: Pediatrics (46.74%), pregnant women (80.55%), Geriatric (49.76%) and other patients (42.99%). Most commonly prescribed antibiotic combinations were Amoxicillin-Clavulanate (3.63%) in oral formulation, Piperacillin-Tazobactam (4.63%) and Sulbactam- Cefoperazone (2.38%) in parenteral formulation. DOT calculation was done for pediatric patients which revealed association of days of therapy with therapeutic outcome. The PDD/DDD ratio revealed more sub use of antibiotics, followed by overuse and least optimal drug utilization. Prescriptions for branded antibiotics were more (81.13%) when compared to generics. Based upon AWaRe classification of antibiotics majority of antibiotics were from Watch group (73.63%). Cost comparison studies showed branded antibiotics are costlier than their alternative generic counterparts with a total mean difference of ₹665.40.
Conclusion: The study indicates that there is lot of scope of improvement in prescribing pattern of antibiotics when practicing rational drug use. Optimized antibiotic prescription is required in geriatric, pediatric and pregnant women, to prevent overuse and subuse of antibiotics in order to prevent bacterial resistance and adverse drug reaction associated with inappropriate antibiotic usage. More of Generic antibiotics should be prescribed and dispensed to reduce the cost burden on patients. Parenteral therapy should be prescribed only when necessary. Culture and sensitivity tests should be mandatory for antibiotics prescription to get more appropriate therapeutic outcome.
Keywords
Antibiotics; AWaRe; DOT calculation; DUE; Modified Kuppuswamy scale 2020; WHO PDD/DDD ratio; Vulnerable population
Introduction
Antibiotic misuse and overuse are biggest concern and threat in a population causing unnecessary expenditure, unwarranted side effects and development of antibiotic resistance thus impacting many aspects of public health. It has been found that in many parts of the world prescription of antibiotics is irrational which causes poor treatment outcomes, increased mortality, longer stay in hospitals and increased cost of treatment. Antibiotics are the highly prescribed drug all over the world and are found almost in each and every prescription. Differences in antibiotic prescriptions were found not only between different countries but also at a regional level. The examples of irrational medications are polypharmacy, self-medication, injectables overuse, inappropriate use of antibiotics and prescribing medicines without set guidelines.
Considering optimal use and antimicrobial resistance, WHO classifies antibiotics into: Access (A), Watch (Wa) and Reserve (Re) groups (AWaRe). Access group has antibiotics such as amoxicillin, benzathine penicillin, trimethoprim- sulfamethoxazole, amoxicillin-clavulanic acid, cloxacillin, which can be used as first and second choice in common infections and have less resistance potential. Watch group has antibiotics such as third generation Cephalosporins, fluoroquinolones and carbapenem, which can be used in specific infections and have high resistance potential. Reserve group has antibiotics which have to be used as last resort for multi-drug resistant organisms and this includes antibiotics like colistin, polymyxin B, fosfomycin, linezolid, and fourth and fifth generation Cephalosporins [1]. Prescribers should follow AWaRe classification for optimal antibiotic use.
Drug utilization evaluation (DUE) is a tool for measuring the drug use appropriateness in hospitals [2]. It is criteria based ongoing, planning and systemic process for monitoring and evaluating the prophylactic, therapeutic and empiric use of drugs. This helps in assuring that the drugs are used in safe and effective manner. Drug utilization evaluation can be used to improve rationality because it helps in monitoring the drug efficacy, cost constraints and other factors related to patient safety.
Vulnerable populations include people who are economically weak, racial and ethnic minorities, the uninsured, low income children, the elderly, the homeless, those with human immunodeficiency virus (HIV), and those with other chronic health conditions, including severe mental illness. Their vulnerability is increased by age, sex and factors such as income, poverty and improper education [3]. Antibiotics should be given with utmost care in pediatrics, geriatrics and in pregnant women.
PDD (Prescribed Daily Dose) is the average daily dose of the drug actually prescribed and DDD (Defined Daily Dose) is the average maintenance dose of the drug per day. DDDs are only assigned for a drug which are given ATC codes and is assigned for adults. If there is no discrepancy between PDD and DDD then the dose of the antibiotic becomes optimal but this does not happen generally.
Prescribers should have an ideal prescribing habit such as: clearly defining the patient’s problem, fixing a proper therapeutic objective, selecting specific medicines by going into detailing of each medicine’s dosage, also considering non pharmacological therapies, proper patient counseling by giving instruction of drug intake, regular evaluation of therapy, prescribing less costly drugs and reducing prescription errors [4].
The objectives of this study were to assess the prescribing patterns of antibiotics in the vulnerable populations who are at high risk because of their age, socio economic status and comorbid conditions by monitoring, evaluating and suggesting any modifications in prescribing habits of healthcare professionals so that medical care can be made rational and cost effective.
Materials and Methods
This was a prospective study which included 551 patients from a selected tertiary care hospital of Andhra Pradesh. This study was carried out from February 10, 2020 to December 9, 2021. Both male and female in-patients under antibiotics therapy of different vulnerable populations such as, pediatric (<18 years, n=139), geriatric (>60 years, n=116), pregnant women (18-40 years, n=58) and other patients (18 to 60 years, n=238) were included in the study. “Other” patients here mean the patients who are chronically, critically, mentally or economically compromised. The Modified Kuppuswamy socio-economic status scale 2020 was used to measure socio-economic status of patients. The scale has five classes which are as follows: Upper class (I) (score 26-29), Upper middle class (II) (score 16 to 25), Lower middle class (III) (score 11 to 15), Upper lower class (IV) (score 5-10) and Lower class (V) (score <5) [5]. Based on this scale our study population was under lower middle class, upper lower class and lower class. Data was collected from the case sheets of individual patients from the hospital on a specially designed data collection form. All antibiotics prescribed were recorded with their dose, route, and dosage form, frequency of administration, indications and duration of therapy. The PDD was divided by WHO DDD to calculate and determine dose utilization discrepancy. This ratio suggests optimal drug utilization when PDD/DDD=1, drug sub use when PDD/DDD <1.0 and drug overuse when PDD/DDD >1.0 [6]. Assigning DDDs in pediatrics is challenging due to variation in body weights. Therefore, days of therapy (DOT) was used [7]. This was associated with therapeutic outcome (cured and not improved) Cost comparison was done between branded and their alternative generic drugs (if it would have been prescribed) and total cost spent on antibiotics during the entire hospitalization was determined. WHO’s AWaRe classification of antibiotics was used to observe choice of antibiotics by the prescribers. PDD/DDD method of WHO was used to measure the antibiotic usage and consumption [8]. Statistical analysis was done using JMP® Pro version 13.0.0 (SAS institute Inc.) and Microsoft® Excel® 2016 MSO (Version 2204). Cost of branded antibiotics was calculated using India Drug Index (Offline Dictionary) version 2.4 di and of generic antibiotics was calculated using Jan Ausadhi Sugam (BPPI) version 5.20.0. Drug information such as dosage, frequency, route of administration, dosage form and duration of treatment was obtained from IBM Micromedex ® Web Applications Access.
The study was approved by respective Institutional Ethics Committee (IEC/IRB ref no:650-A-EC/650-A-02/20). All the study participants were informed about study details and informed consents were obtained. All necessary permissions were obtained from the hospital authorities for hospital record collection, review and analysis. Our study was initiated after ethics committee clearance.
Results
Among 551 patients, 282 (51.8%) were male patients and 269 (48.82%) were female patients and the mean age in years were found as: 12 ± 4.51 among pediatrics, 29 ± 7.03 among pregnant women, 69 ± 6.65 among geriatrics and 42 ± 11.46 among other vulnerable patients.
It was observed that total parenteral antibiotics were prescribed more (55%) when compared with oral dosage forms (Table 1). Percentage of parenteral (P) antibiotics should be reduced and has to be given only when necessary or when intended because parenteral dosage forms are costlier when compared to oral (O) dosage forms and they also cause patient discomfort.
Table 1: Distribution based on antibiotic dosage forms.
| Parameters | Vulnerable population group | Chi square test at 0.05 level of significance | ||||
|---|---|---|---|---|---|---|
| Pediatric | Pregnant women | Geriatrics | Others | |||
| Antibiotics dosage form (excluding 4 ointments) (N=796) | Parenteral (n=440) | 105 (23.86%) | 53 (12.05%) | 88 (20.00%) | 194 (44.09%) | P value <0.0001 |
| Oral (n=356) | 75 (21.07%) | 19 (5.34%) | 121 (3.37%) | 141 (39.61%) | ||
Therapeutic outcome was observed in the population and it was found that 487 patients got cured (129 in pediatric, 55 in pregnant women, 95 in geriatric and 208 in “other” group). One way ANOVA for cured and not improved patients was performed in the vulnerable population which shows F distribution (0.0185) which is significant at 0.05 level of significance. To determine which group is significantly different, a Post hoc (Tukey-Kramer test) was performed at 0.05 level of significance. The result showed that the means of geriatric group is significantly different from pediatric, pregnant women and other groups (Figure 1).
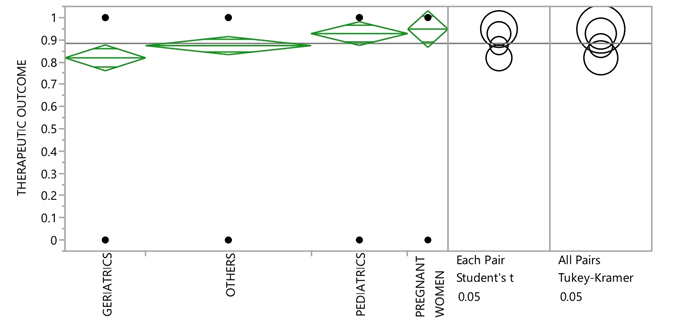
Figure 1: One way ANOVA for therapeutic outcome among vulnerable population.
It was observed that among the total prescription (N=551), no. of prescriptions of branded antibiotics was found to be 447 whereas the no. of prescriptions of generic antibiotics were only 104 (Figure 2). A chi square test was performed for the type of prescription among the different vulnerable groups and it was found to be significant at 0.05 level of significance (Table 2).
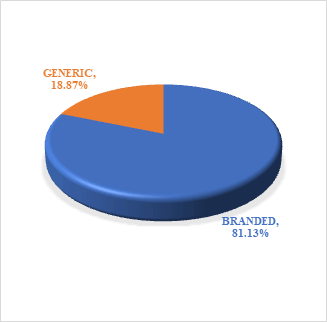
Figure 2: Overall distributionn of branded and generics antibiotic prescription in the study population.
Table 2: Number of branded and generic antibiotic prescription in each study population.
| Vulnerable group | Brands (n=447) | Generics (n=104) | |
|---|---|---|---|
| Geriatrics | 85 (19.02%) | 31 (29.81%) | Pearson value: 0.0343 |
| Others | 203 (45.41%) | 35 (33.65%) | |
| Pediatrics | 115 (25.73%) | 24 (23.08%) | |
| Pregnant women | 44 (9.84%) | 14 (13.46%) |
Out of 551, 520 patients were subjected to culture sensitivity test and among these for 59 patients’ empirical treatment was changed based upon the culture sensitivity test report whereas for remaining patients (461), the empiric antibiotic treatment was continued (Figure 3). After receiving the culture sensitivity reports, the antibiotics were either removed (de-escalated) or a new antibiotic was added (escalated) among those 59 patients (Figure 4).
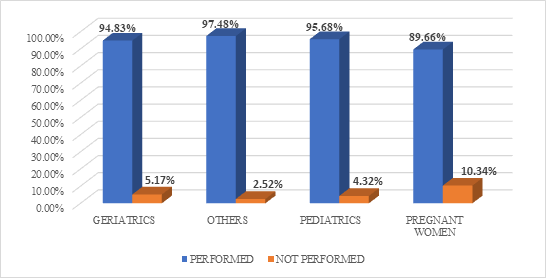
Figure 3: Distribution based on culture sensitivity testing.
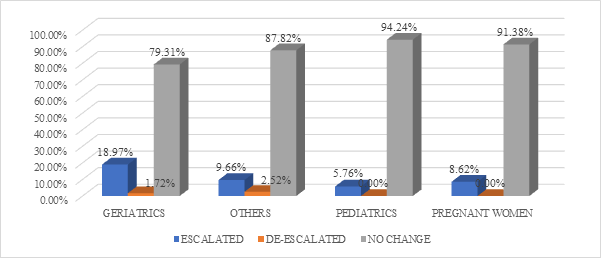
Figure 4: Distribution based on changes made in antibiotic prescription after culture sensitivity test.
Decision Tree, Figures 5 and 6 reveals cost comparison study between the prescribed branded antibiotics and their alternative generic antibiotics and it was found that branded antibiotics were costlier than alternative generic antibiotics if it was prescribed. Highest difference can be observed among geriatric patients. Overall mean difference in cost was measured between branded and alternative generic drugs in the vulnerable population and it was found to be ₹665.40.
As observed in Table 3, most prescribed antibiotics in pediatrics were ceftriaxone, cefixime and amoxiclav. In pregnant women most prescribed antibiotics were cefixime, ceftriaxone, cefotaxime and metronidazole, the commonly prescribed antibiotics in geriatrics were cefixime, azithromycin and ceftriaxone and the antibiotics prescribed in other vulnerable patients were ceftriaxone and azithromycin. Most commonly used antibiotic class among all the vulnerable population was Cephalosporins followed by macrolides. In Cephalosporins, third generation Cephalosporins (cefixime, ceftriaxone, cefotaxime, cefoperazone and cefpodoxime) were widely prescribed and in few cases, cefuroxime belonging to second generation of cephalosporin were prescribed. Cephalosporins were widely used in combination with azithromycin, doxycycline, sulbactam, metronidazole, amikacin in various indications in the study population. Most commonly prescribed antibiotic combination among all study population was Amoxicillin- Clavulanate in oral formulation and Piperacillin-Tazobactam, Sulbactam-Cefoperazone in parenteral formulation.
Table 3: Choice of antibiotic prescription in the study group.
| Antibiotic class | Antibiotics | Number of prescriptions | ||||
|---|---|---|---|---|---|---|
| Dosage form and AWaRe group | Pediatrics | Pregnant women | Geriatrics | Others | Total | |
| Glycopeptides | Vancomycin(P)(Wa) | 5(2.72%) | 5 (0.63%) | |||
| Aminoglycosides | Amikacin(P)(A) | 6(3.26%) | 2(2.78%) | 2(0.96%) | 14(4.18%) | 24 (3%) |
| Gentamicin(P)(A) | 5(6.94%) | 4(1.19%) | 9 (1.13%) | |||
| Penicillin-Betalactamase Inhibitors | Amoxicillin-Clavulanate(O)(A) | 20(10.87%) | 2(2.78%) | 7(2.09%) | 29 (3.63%) | |
| Piperacilin+Tazobactzm (P)(Wa) | 4(2.17%) | 20(9.57%) | 13(3.88%) | 37 (4.63%) | ||
| Macrolides | Azithromycin(O)(Wa) | 3(1.63%) | 46(22.01%) | 49(14.63%) | 98 (12.25%) | |
| Cephalosporins | Cefixime(O)(Wa) | 20(10.87%) | 14(19.44%) | 52(24.88%) | 37(11.04%) | 123 (15.38%) |
| Cefotaxime(P)(Wa) | 15(20.83%) | 3(0.90%) | 18 (2.25%) | |||
| Ceftriaxone(P)(Wa) | 66(35.87%) | 27(37.50%) | 46(22.01%) | 101(30.15%) | 240 (30%) | |
| Cefuroxime(O)(Wa) | 2(2.78%) | 2 (0.25%) | ||||
| Cefpodoxime(O)(Wa) | 6(2.87%) | 3(0.90%) | 9 (1.13%) | |||
| Fluroquinolones | Ciprofloxacin(O)(Wa) | 2(1.09%) | 2 (0.25%) | |||
| Ofloxacin(O)(Wa) | 9(4.89%) | 9 (1.13%) | ||||
| Ciprofloxacin(P)(Wa) | 1(0.48%) | 7(2.09%) | 8 (1%) | |||
| Levofloxacin(O)(Wa) | 5(2.39%) | 8(2.39%) | 13 (1.63%) | |||
| Oxazolidinones | Linezolid(O)(Re) | 3(1.63%) | 3(0.90%) | 6 (0.75%) | ||
| Carbapenems | Meropenem(P)(Wa) | 5(2.72%) | 2(0.96%) | 2(0.60%) | 9 (1.13%) | |
| Faropenem(O)(Re) | 3(1.44%) | 2(0.60%) | 5 (0.63%) | |||
| Nitroimidazoles | Metronidazole(P)(A) | 2(1.09%) | 4(5.56%) | 16(7.66%) | 33(9.85%) | 55 (6.88%) |
| Ornidazole(O)(A) | 9(4.89%) | 9 (1.13%) | ||||
| Tetracyclines | Doxycycline(P)(A) | 16(8.70%) | 16 (2%) | |||
| Doxycycline(O)(A) | 1(1.39%) | 5(2.39%) | 20(5.97%) | 26 (3.25%) | ||
| Carboxylic Acid | Mupirocin(Ointment) | 4(2.17%) | 4 (0.5%) | |||
| Betalactamase Inhibitors-Cephalosporins | Sulbactam-Cefoperazone(P) | 1(0.54%) | 1(0.48%) | 17(5.07%) | 19 (2.38%) | |
| Sulphonamides | Sulfamethoxazole-Trimethoprim(O)(A) | 9(4.89%) | 9 (1.13%) | |||
| Rifamycin Derivative | Rifaximin(O)(Wa) | 4(1.91%) | 12(3.58%) | 16 (2%) | ||
| Total | 184 | 72 | 209 | 335 | 800 | |
The drug utilization was determined by PDD/DDD ratio of antibiotics in different study population i.e., pregnant women, geriatric patients and other vulnerable groups (Table 4). The result of PDD/DDD suggests that there is high rate of sub use which may affect the therapeutic effect and overuse which implies drug abuse and this shows discrepancy between PDD and DDD.
Table 4: Antibiotics utilization among pregnant women, geriatrics and others, based on PDD/DDD ratio.
| Category | Dosage form | Antibiotics | ATC code | PDD | DDD | PDD/DDD | Utilization |
|---|---|---|---|---|---|---|---|
| Pregnant women | Parenteral | Amikacin | J01GB06 | 750 | 1000 | 0.75 | Sub-use |
| Ceftriaxone | J01DD01 | 1000 | 2000 | 0.5 | Sub-use | ||
| Cefotaxime | J01DD04 | 2000 | 4000 | 0.5 | Sub-use | ||
| Oral | Cefixime | J01DD08 | 400 | 400 | 1 | Optimal | |
| Amoxicillin-Clavulanate | J01CR02 | 1250 | 1500 | 0.83 | Sub-use | ||
| Cefuroxime | J01DC02 | 1000 | 500 | 2 | Overuse | ||
| Doxycycline | J01AA02 | 200 | 100 | 2 | Overuse | ||
| Geriatrics | Parenteral | Amikacin | J01GB06 | 500 | 1000 | 0.5 | Sub-use |
| Cefotaxime | J01DD01 | 2000 | 4000 | 0.5 | Sub-use | ||
| Ceftriaxone | J01DD04 | 2000 | 2000 | 1 | Optimal | ||
| Ciprofloxacin | J01MA02 | 1000 | 850 | 1.18 | Overuse | ||
| Meropenem | J01DH02 | 3000 | 3000 | 1 | Optimal | ||
| Metronidazole | J01XD01 | 1500 | 1500 | 1 | Optimal | ||
| Piperacillin-Tazobactam | J01CR05 | 6750 | 14000 | 0.48 | Sub-use | ||
| Sulbactam-Cefoperazone | J01DD62 | 3000 | 4000 | 0.75 | Sub-use | ||
| Oral | Cefpodoxime clavulanate | J01DD13 | 650 | 400 | 1.63 | Overuse | |
| Azithromycin | J01FA10 | 500 | 300 | 1.67 | Overuse | ||
| Doxycycline | J01AA02 | 200 | 100 | 2 | Overuse | ||
| Faropenem | J01DI03 | 600 | 750 | 0.8 | Sub-use | ||
| Levofloxacin | J01MA12 | 1000 | 500 | 2 | Overuse | ||
| Cefixime | J01DD08 | 400 | 400 | 1 | Optimal | ||
| Rifaximin | A07AA11 | 1100 | 600 | 1.83 | Overuse | ||
| Others | Parenteral | Ceftriaxone | J01DD04 | 1000 | 2000 | 0.5 | Sub-use |
| Amoxicillin-Clavulanate | J01CR02 | 1200 | 3000 | 0.4 | Sub-use | ||
| Amikacin | J01GB06 | 500 | 1000 | 0.5 | Sub-use | ||
| Ciprofloxacin | J01MA02 | 400 | 800 | 0.5 | Sub-use | ||
| Cefotaxime | J01DD01 | 1000 | 4000 | 0.25 | Sub-use | ||
| Sulbactam-Cefoperazone | J01DD62 | 1500 | 4000 | 0.38 | Sub-use | ||
| Metronidazole | J01XD01 | 500 | 1500 | 0.33 | Sub-use | ||
| Piperacillin-Tazobactam | J01CR05 | 4500 | 14000 | 0.32 | Sub-use | ||
| Gentamycin | J01GB03 | 240 | 240 | 0.33 | Optimal | ||
| Meropenem | J01DH02 | 1000 | 3000 | 0.33 | Sub-use | ||
| Oral | Cefixime | J01DD08 | 200 | 400 | 0.5 | Sub-use | |
| Doxycycline | J01AA02 | 100 | 100 | 1 | Optimal | ||
| Rifaximin | A07AA11 | 1200 | 600 | 0.92 | Overuse | ||
| Cefpodoxime | J01DD13 | 650 | 400 | 1.63 | Overuse | ||
| Amoxicillin-Clavulanate | J01CR02 | 1250 | 1500 | 0.83 | Sub-use | ||
| Levofloxacin | J01MA12 | 750 | 500 | 1.5 | Overuse |
There was maximum overuse of oral antibiotics in geriatric patients, in pregnant women there was maximum sub use of parenteral antibiotics (amikacin, cefotaxime and ceftriaxone) and oral amoxicillin-Clavulanate and overuse of oral cefuroxime and doxycycline whereas in other patients there was mainly sub use of parenteral and oral antibiotics except oral levofloxacin which was overused. (Figure 7)
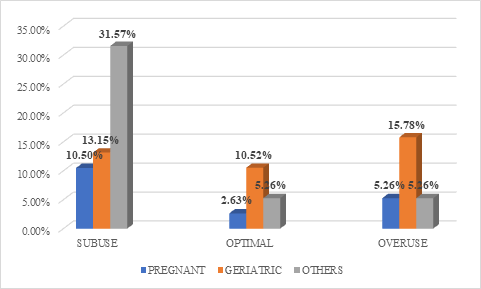
Figure 7: Drug utilization based on PDD/DDD ratio.
Children are considered to be most vulnerable population [9]. Usage of antibiotics in pediatric patients were measured by DOT calculation (Table 5) and it was found that patients who were under antibiotic therapy for less than 5 days had a greater cure percentage as compared to those on antibiotic therapy for 5 and more than 5 days. Based on Fisher’s Exact test, probability (p value: 0.0075) of cured patients was greater for short term (<5 days) treatment than long term treatment (≥ 5 days).
Table 5: DOT analysis for antibiotics utilization among pediatric patients.
| DOT (in days) | Not improved | Cured | Total |
|---|---|---|---|
| <5 | 0 | 52 (40.31%) | 52 (37.41%) |
| ≥ 5 | 10 (100%) | 77(59.69%) | 87 (62.58%) |
| Total | 10 (7.19%) | 129 (92.81%) | 139 |
Discussion
In this study we observed that, the average number of drugs prescribed to each patient was 4.15 including antibiotics. Such polypharmacy increases the chances of side effects, adverse drug reactions, drug interactions, bacterial resistance and cost burden. Management of infection in geriatrics is challenging due to comorbid conditions, polypharmacy and pharmacokinetic and pharmacodynamics changes which puts them on high risk of drug drug interactions among antibiotics and between antibiotics and other medicines making medicines less effective, causing serious side effects or increasing/decreasing the action of particular medicines [10,11]. The mean therapeutic outcome of geriatric patients was lesser than the mean of response (0.88) whereas the means of pediatric, pregnant women and other groups were either closer or above the mean of response (Figure 1).
As observed in Figure 5 maximum cost of branded antibiotics scaled up to Rupees 25,000 whereas its generic alternative will cost up to Rupees 4,000 (Figure 6) if it had been prescribed. Whenever generic drugs were prescribed to the patients, they were dispensed with branded drugs at the pharmacy due to unavailability of generics in the hospital pharmacy. Healthcare professionals must prefer a greater number of generic prescriptions and at the same time the pharmacist should also dispense the same so that cost burden on patients is reduced. Large number of branded prescriptions is highly influenced by aggressive brand promotions by various pharmaceutical companies to the doctors and chemists.
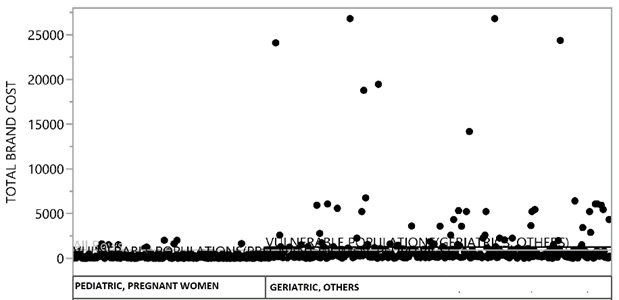
Figure 5: Mean difference of total cost of branded antibiotics in pediatric and pregnant women was 266.94±361.47 whereas for geriatric and other group was 1262.52±3276.33.
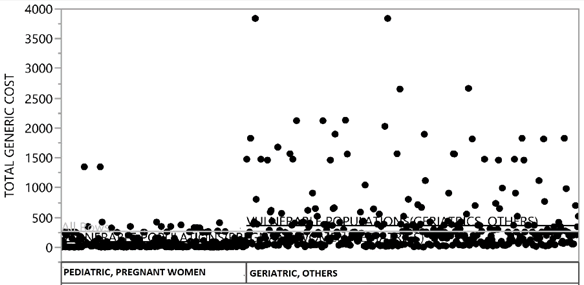
Figure 6: Mean difference of total cost of generic antibiotics in pediatric and pregnant women was 92.06±162.98 whereas for geriatric and other group was 362.63±541.90.
Many of the antibiotics were prescribed before the availability of culture sensitivity reports and in many cases, specimens were sent for culture sensitivity test after a few days of empirical antibiotics treatment. Whenever empiric therapy is to be initiated, broad spectrum antibiotics should be the drug of choice [12]. Sub use of antibiotics may lead to bacterial resistance and overuse of antibiotics may lead to risk of adverse effects. Antibiotic resistance increases health care cost, severity of disease and death rate due to disease. The more overuse of oral antibiotics in geriatrics can be a concern because as a person ages the gastrointestinal tract undergoes changes causing delayed gastric emptying, reduced gastrointestinal blood flow and alterations in pH leading to decreased dissolution, absorption and bioavailability of drugs, also there is increased proportion of adipose tissue and decreased lean body mass in geriatrics leading to increased distribution of lipid soluble parenteral drugs and decreased distribution of water soluble parenteral drugs respectively, hence parenteral should also be prescribed with lot of precautions in geriatrics [13]. Overuse of antibiotics also leads to more economic burden on geriatric patients who have limited source of income and are dependent on others. The more subuse of antibiotics in pregnancy can be because of using lowest effective dose so that risk to fetal development can be reduced [14]. The other reason can be less plasma protein binding of drugs in pregnancy due to low levels of albumin and alpha 1-acid glycoprotein which might lead to high concentration of free drugs which can cause drug related toxicity [15]. An excess use of Watch (Wa) group of antibiotics based upon WHO’s AWaRe was observed and because of this, there can be high potential of antimicrobial resistance [16]. Decrease in cure percentage of pediatric patients was observed in long term (≥ 5 days) treatment. This could be due to inappropriate prediction and choice of antibiotics and also because of delayed culture sensitivity testing. In the study it was found that pediatric doses were given based upon patient body weight which is a good practice. Though the hospital lacked the approved list of essential medicines, 86% of drugs were mentioned in the essential drug lists were present in the pharmacy. Prescription of drugs from essential drug lists costs lesser; hence doctors should prescribe antibiotics from essential drug list [17].
Conclusion
This study on drug utilization evaluation tries to provide some insight into the efficiency of antibiotic use based upon ideal prescription. The study provides an impression that there is lot of improvement required in prescribing pattern of antibiotics when practicing rational drug use. WHO’s AWaRe classification of antibiotics has to be followed judiciously for optimal drug use and to reduce antimicrobial resistance by shifting the prescription from Watch group to Access group of antibiotics wherever possible. Optimized antibiotic prescription is required in geriatric, pediatric and pregnant patients to prevent overuse and subuse of antibiotics in order to prevent bacterial resistance and adverse drug reaction associated with inappropriate antibiotic usage and also to increase the therapeutic outcome. This can be achieved by reducing the discrepancy between PDD and DDD by making PDD/DDD quotient 1 or close to 1. Culture and sensitivity tests should be mandatory for antibiotics prescription. The average number of drugs on a prescription has to be reduced to control side effects, adverse drug reactions, drug interactions, bacterial resistance and cost burden. Parenteral should be prescribed only when absolutely necessary. Doctors can improve antibiotic prescribing by using shortest and effective duration of therapy by choosing proper antibiotic and also re-assessing the treatment based upon diagnostic test reports. Healthcare professionals should focus on continuous medical education to have better clinical outcome in their daily practices and prescription of medicines should be evidence based. Prescribing generic antibiotics should be the priority for cost containment and similarly pharmaceutical companies should also rationalize cost of existing drugs/new drugs.
Acknowledgements
The authors would like to gratefully acknowledge all cooperation and support from the patients and hospital administration for facilitating this study.
Source of Funding
None.
Conflict of Interest
The authors have no conflicts of interest regarding this study.
References
- J. Yin, H. Li, Q. Sun, Analysis of Antibiotic consumption by aware classification in shandong province, China, 2012–2019: A panel data analysis, Front Pharmacol, 12 (2021), 790817.
[Crossref] [Google Scholar] [PubMed]
- S. Mousavi, M. Behi, M.R. Taghavi, A. Ahmadvand, S.Ziaie, et al. Drug utilization evaluation of imipenem and intravenous ciprofloxacin in a teaching hospital, Iran J Pharm Res, 12(2013), 161-167.
[Google Scholar] [PubMed]
- Analysis of Antibiotic consumption by aware classification in shandong province, China, 2012–2019: A panel data analysis
- M. Pollock, O.V. Bazaldua, A.E. Dobbie, appropriate prescribing of medications: an eight-step approach, Am Fam Physician, 75(2007), 231-236.
[Google Scholar] [PubMed]
- S.M. Saleem, Modified Kuppuswamy socioeconomic scale updated for the year 2020, Indian J Forensic and Community Med, 7(2020), J2020.
- R. Sánchez-Huesca, A. Lerma, R.M.E Guzmán-Saldaña, C. Lerma, Prevalence of antibiotics prescription and assessment of prescribed daily dose in outpatients from Mexico City, Antibiotics, 9(2020), 38.
[Crossref] [Google Scholar] [PubMed]
- V. Schechner, E. Temkin, S. Harbarth, Y. Carmeli, M.J. Schwaberb, Epidemiological interpretation of studies examining the effect of antibiotic usage on resistance, Clin Microbiol Rev, 26(2013), 289-307.
[Crossref] [Google Scholar] [PubMed]
- M. Sharma, A. Damlin, A. Pathak, C.S. Lundborg, Antibiotic prescribing among pediatric inpatients with potential infections in two private sector hospitals in central India, PLOS ONE, 10(2015).
[Crossref] [Google Scholar] [PubMed]
- P.D. Pietro, O.D.C. Alberighi, M. Silvestri, M.A. Tosca, A. Ruocco, et al. Monitoring adherence to guidelines of antibiotic use in pediatric pneumonia: the MAREA study, Ital J Pediatr, 43(2017), 113.
[Crossref] [Google Scholar] [PubMed]
- C.L. Beckett, S. Harbarth, B. Huttner, Special considerations of antibiotic prescription in the geriatric population, Clin Microbiol Infect, 21(2015).
[Crossref] [Google Scholar] [PubMed]
- A. Dylis, A.S. Boureau, A. Coutant, E. Batard, F. Javaudin, et al. Antibiotics prescription and guidelines adherence in elderly: impact of the comorbidities, BMC Geriatr, 19(2019).
[Crossref] [Google Scholar] [PubMed]
- S. Leekha, C.L. Terrell, R.S. Edson, General principles of antimicrobial therapy, Mayo Clin Proc, 86(2011), 156–167.
[Crossref] [Google Scholar] [PubMed]
- A. Giarratano, S.E. Green, D.P. Nicolau, Review of antimicrobial use and considerations in the elderly population, Clin Interv Aging, 13 (2018), 657-667.
[Crossref] [Google Scholar] [PubMed]
- E.R. Norwitz, J.A. Greenberg, Antibiotics in pregnancy: Are they safe? Rev Obstet Gynecol, 2(2009), 135-136.
[Google Scholar] [PubMed]
- M. Feghali, R. Venkataramanan, S. Caritis, Pharmacokinetics of drugs in pregnancy, Semin Perinatol, 39(2015),512-9.
[Crossref] [Google Scholar] [PubMed]
- S. Gandra, A. Kotwani, Need to improve availability of “access”group antibiotics and reduce the use of “watch” group antibiotics in India for optimum use of antibiotics to contain antimicrobial resistance, J Pharm Policy Pract, 12 (2019), 20.
[Crossref] [Google Scholar] [PubMed]
- M.S. Taglione, H. Ahmad, M. Slater, B. Aliarzadeh, R.H. Glazier, et al. Development of a preliminary essential medicines list for Canada, CMAJ OPEN, 5(2017), E137-E143.
[Crossref] [Google Scholar] [PubMed]
Copyright: © 2022 Amit Kumar, et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.

