Research Article: Journal of Drug and Alcohol Research (2023) Volume 12, Issue 6
Correlation between Risk Factors and Demographical Factors of Colorectal Cancer: An Observational Cohort Study
Shiv Shankar Shah, Swathi Putta and Eswar Kumar Kilari*Eswar Kumar Kilari, Department of Pharmacology, AU College of Pharmaceutical Sciences, India, Email: ekilari@gmail.com
Received: 03-Jul-2023, Manuscript No. JDAR-23-104879; Editor assigned: 05-Jul-2023, Pre QC No. JDAR-23-104879 (PQ); Reviewed: 19-Jul-2023, QC No. JDAR-23-104879; Revised: 24-Jul-2023, Manuscript No. JDAR-23-104879 (R); Published: 31-Jul-2023, DOI: 10.4303/JDAR/236250
Abstract
Genetic and environmental factors play an important part in the etiology of colorectal cancer. The majority of colorectal cancers are sporadic; approximately three-quarters of patients have a negative family history. It was an observational cohort study, a total of 182 patients with colorectal cancer of any stage were enrolled in this observational study. Data were collected retrospectively and prospectively over 3 years to correlate demographical factors and colorectal cancer and its progression. The study outcomes suggested that demographical factors are influenced the risk of colorectal cancer and care must be taken while in the therapy of colorectal cancer.
Keywords
Colorectal cancer; Demographical factors; Risk factors
Introduction
Colorectal cancer is the third most common cancer in men and the second most common cancer in women. It accounts for 10% of all cancers and 8% of cancer-related deaths. Treatment at earlier stages can reduce the mortality and morbidity of colorectal cancer. Although the incidence of colon cancer in young adults is increasing, only 1.6% of all colon cancers are diagnosed in patients aged 35 years and younger. By 2030, the incidence of colorectal cancer will increase by 90% and 124.2% in patients aged 20 and 34 years, respectively.
Focusing on causes and risk factors will also help researchers uncover the underlying biology of early-onset colorectal cancer. More specifically, it may help scientists pinpoint the specific molecules that control the growth of colorectal cancer in young people which in turn could lead to new ideas for colorectal cancer screening and treatment. Developmental and biological differences between colorectal cancer varieties may reflect different susceptibility to neoplastic transformation, and these differences may explain different pathogenetic mechanisms between the diseases.
The 5-year relative survival rate for localized-stage colorectal cancer is 91%. About 37% of patients are diagnosed at this early stage. If the cancer has spread to surrounding tissues or organs and/or the regional lymph nodes, the 5-year relative survival rate is 73%. About 36% of patients are diagnosed at this regional stage. If the cancer has spread to distant parts of the body, the 5-year relative survival rate is 14%. About 22% of patients are diagnosed at this late stage.
The purpose of this study is to investigate the statistically significant correlation of epidemiological, clinical, histological, and pathological characteristics, as well as the differences between them in terms of periods of disease progression, taking into account the targeted treatment administered.
Materials and Methods
A total of 182 patients with colorectal cancer of any stage were enrolled in this observational study. Data were collected retrospectively and prospectively over 3 years. The correlation was done to the selected modifiable and non-modifiable risk factors with the clinicopathology of colorectal cancer. The age, gender, and tumour location are selected as risk factors to correlate with epidemiological and clinicopathological risk factors of colorectal cancer survivors. The observational cohort study was conducted in the Oncology department, at King George Hospital, Visakhapatnam. The Institutional Ethics Committee (IEC) of King George Hospital (Regd No. ECR/197/Inst/ KGH/2013/DCGI/20-04-2013) approved the protocol. The required data was obtained from the medical records databases that were searched to retrieve the records of patients who were diagnosed with advanced colorectal cancer with local progression or distant metastasis and who underwent first-line systemic chemotherapy for advanced colorectal cancer between February 1, 2019, and August 31, 2022.
Inclusion criteria
All patients with a provisional diagnosis of colorectal malignancies attending the Department of Oncology, Subjects who are between the age of 25 years-80 years.
Exclusion criteria
The patients below 25 years and those with bleeding from the rectum due to benign polyps, benign ulcers, inflammatory bowel disease, diverticulosis, and subjects below the age of 25 years. The subjects who are diagnosed only with caecum abnormalities, splenic, and pancreatic abnormalities, pregnant women, breastfeeding women, and COVID-19 positive subjects were excluded from the study. Patients who had incomplete medical records or died from causes other than cancer were excluded from the study group.
Statistical Analysis
Data were entered in an Excel spreadsheet for Windows and analyzed using GraphPad Prism 9. Data was distributed according to the parameters selected; categorical variables were presented as percentages (%). The correlations of the selected factors were analyzed using multivariate analysis, correlation matrix with Pearson r correlation at 95% confidence interval and p-value was calculated using two-tailed. The considered p-value is at p>0.05.
Results and Discussion
The number of elderly patients with colorectal cancer is expected to escalate in the coming years. This escalation will increase the burden on health systems nationally and globally. The age-standardized mortality rate for men is 50% higher than for women. It is challenging to determine how much of the sexual dimorphism in CRC mortality can be attributed to gender differences in CRC incidence. Improvements in the selection and management of elderly patients with colorectal cancer may improve outcomes and optimize the use of healthcare resources. 70% of these patients are over 65 years of age and 21% are even over 80 years old. Colon cancer is uncommon before age 40; the incidence begins to increase significantly between the ages of 40 and 50, and age-specific incidence rates increase with each subsequent decade. Some registries report a rising incidence of CRC even among young adults up to 39 years of age, although the absolute number of cases in this age group remains far lower than in adults aged 50 and over [1]. Several retrospective studies have shown that female CRC patients have a longer survival rate than male patients. For example, a German population-based cohort study involving 185,967 patients showed that women had significantly better overall and recurrence-free survival than men [2]. A 2017 meta-analysis of 37 clinical trials showed that women had better overall and cancer-specific survival than men [3]. This study indicated that the incidence is more in men than in women, it may be due to many protective factors in women, which men are related to hormonal differences, and it was observed more in the age group of 51 years-60 years, as shown in Figure 1.
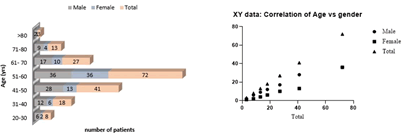
Figure 1: Distribution of study subjects by age and gender and correlation of age and gender
The incidence of CRC was found to be more in men at 51 years-60 years of age. There was a strong correlation between age and gender distribution at a p-value of 0.0001. The null hypothesis was rejected and the alternative was conserved. Studies of the effects of HRT on cancer progression in postmenopausal women attributed a protective role to female sex hormones and encouraged many researchers into the field. Similarly, oral contraceptive use has been reported to reduce the risk of CRC by 10%-20% [4]. Consistent with these findings, oophorectomy and early suppression of female sex hormones have been shown to increase the risk of CRC by 30% [5].
The number of registrations was found to be higher in 2021-2022 than in 2019-20 and 2020-2021. This may be due to the impact of COVID-19 on public health and reduced hospital attendance, so the number of registered cases is lower than in other years. As already said, the incidence of CRC is higher in 51 years-60 years and especially more in 2021-2022.
The number of subjects registered every year was found to be more with the elderly. The current study reported that the age range of 51-60 was found more compared to other age groups in all years 2019-20; 2020-21, and 2021-22. There was a significant correlation between the age and year of registration at all the years at 0.0001 p-values. The null hypothesis was rejected and the alternative was conserved (Figure 2). In this study, the first diagnosis was made 6 years-10 years after exposure to CRC in the selected population. For males, it was aged 6 years-10 years, and for females aged ≥ 11 years. Delayed diagnosis in women aged 51 years-60 years was associated with the premenopausal stage in women. Many studies report that premenopausal women have a better 5-year survival rate than age-matched patients, and younger women (18 years-44 years) have a lower mortality rate over a comparable period compared to older women (over 50) [6]. The early diagnosis also depends on the gender of the subjects. Our data shows that men have a comparatively higher risk of developing colorectal cancer than women and were more after 6 years-10 years of CRC but there was no correlation existed between the first time of diagnosis and age distribution according to Pearson r correlation. The null hypothesis was accepted (Figure 3).
The risk score increased progressively with overweight as estimated by Body Mass Index (BMI), where the risk ranged from 1.79 for a BMI between 22 and 24 to 2.79 for a BMI over 30. A recent linear dose-response meta-analysis of four prospective studies showed that each 5 kg increase in weight in adults was associated with an approximately 6% increased risk of colon cancer [7]. Similarly, another meta-analysis of 30 prospective studies reported an increased risk of colon cancer for every 5-unit increase in BMI in both men and women, and the association was stronger in men [8].
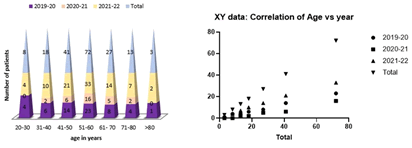
Figure 2: Correlation of age and year of registration and correlation
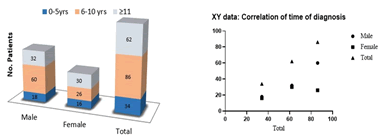
Figure 3: Distribution of study subjects by gender and time of diagnosis
In this study, most of the subjects are 25-29.9, among them more males than females were found. There was a strong significant association between gender and BMI as shown in Figure 4. Some researchers reported that an association exists between the age and BMI of the CRC subjects. A strong correlation is there between gender and BMI at p 0.0005 in men and p 0.0018 in women in this study and the null hypothesis was rejected and the alternative was conserved.
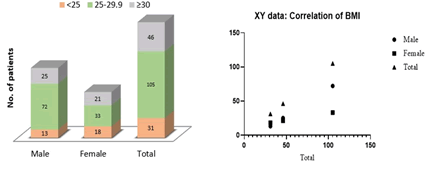
Figure 4: Distribution of study subjects by gender and BMI and correlation
At present, a higher incidence was observed among employees than among employees, especially among men, as shown in Figure 5. Analyzes by anatomical subsite showed an excess risk for those in employment and an increased risk in employed men primarily for cecal cancer. Employment- based on assessment of activity level as high, moderate, or sedentary. Sedentary men had a risk of colon cancer at least 1.6 times higher than men whose jobs required high activity. The risk increased gradually with decreasing activity levels. The protective effect of physical activity was very strong. In the descending colon and descends in a gradient proximally and distally. Findings by occupational physical activity level confirmed recent reports of an increased risk of colon cancer associated with employment in sedentary jobs.
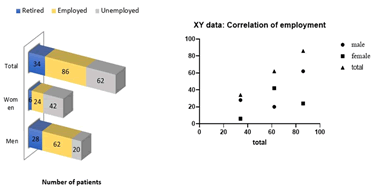
Figure 5: Distribution of study subjects by gender and employment
However, the study showed that there was no correlation between gender and BMI Physical activity is also one of the factors for the CRC survivors, but observed that there was no significant correlation between gender and employment status; the null hypothesis was accepted.
Cigarette smoking is associated with increased incidence and mortality from CRC. A meta-analysis of 106 observational studies estimated that the risk of developing CRC was increased in cigarette smokers compared to never smokers. In this study, distribution was done according to the subjects’ smoking habits and gender. The distribution was according to the never, former, current, and ever. There was a correlation between the men and smoking trend at p 0.0165 according to Pearson r correlation. The null hypothesis was rejected and the alternative was conserved. The distribution of study subjects by location of tumor and smoking habits.
The correlation was found to be more at the right colon in every smoking habit at p 0.0071 and rectosigmoid at 0.0146. The null hypothesis was rejected and the alternative was conserved. Smoking is often associated with the development of colorectal adenomas, its connection with CRC has only been mentioned in recent years. Smoking acts as an initiating agent for CRC, increasing the risk of adenomas after 20 years and cancer after 35 years of dependence. This risk is greater in the right colon [9]. This study is supported by previous reports on the association of smoking with the incidence and progression of CRC. The association with smoking habits is greater in men with a strong correlation in all habits (Figure 6). Among the 182 subjects, 20.88% are with right-sided colon and the correlation is also high with smoking and also related to the duration of smoking (Figure 7). Among the patients, there are more smokers aged 20 years-30 years, and 26.25% have right-sided colon cancer, and the frequency of smoking is also related to the manifestation of the tumor. ≥ 20 smoking habits were observed to be more prone to 36.87% CRC and right-sided CRC was found more common in 46.25% (Figure 8). There was no strong correlation between smoking duration and smoking frequency with CRC. The study revealed that right colon cancer and having 20 years-30 years of smoking habit are more. There was no strong and significant correlation between the duration of smoking and tumor location in the selected subjects. There was no significant correlation between smoking frequencies with the tumor location. The null hypothesis was accepted (Figure 9).
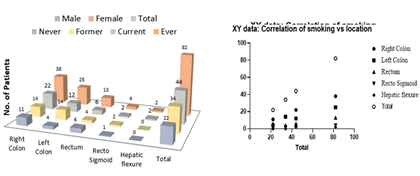
Figure 6: Distribution of study subjects by smoking and location of tumor and correlation
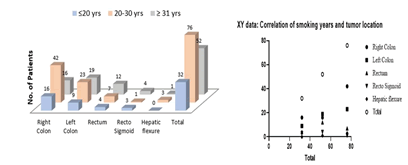
Figure 7: Distribution of study subjects by duration of smoking and location of tumor and correlation
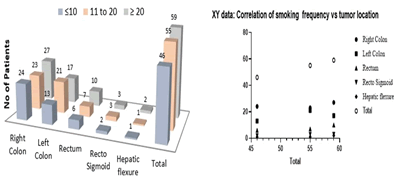
Figure 8: Distribution of study subjects by smoking frequency and location of tumor and correlation
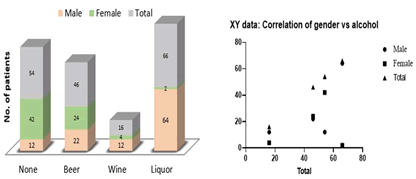
Figure 9: Distribution of study subjects by gender and alcohol consumption and correlation
An association between alcohol consumption and an increased risk of CRC has been observed in several studies. A meta-analysis of 27 cohorts and 34 case-control studies concluded that there was a significant increase in CRC risk in moderate (2 drinks to 3 drinks per day) and heavy drinkers (≥ 4 drinks per day) compared with never-drinkers, but not light drinkers (≤ 1 drink per day) [10]. A pooled analysis of 8 cohort studies from North America and Europe found a slightly increased risk of colorectal cancer (45% for colon cancer and 49% for rectal cancer) in men with regular high alcohol intake (≥ 45 g/day) compared with those whom they don’t drink and women together. The association of alcohol consumption with colorectal cancer risk may be stronger among Asian populations compared with Western populations. Researchers suggested a stronger positive association of moderate and heavy alcohol drinking with cancer in the distal colon compared to cancer in the proximal colon, but the difference was not statistically significant [10].
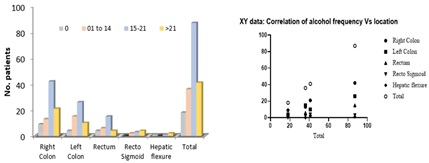
Figure 10: Distribution of study subjects by alcohol quantity and location of tumor and correlation
The distribution by gender and alcohol consumption was done and it was observed that among the subjects, liquor consumption, beer, and none. But overall consideration there was no significant correlation between alcohol consumption and CRC at p>0.05 (Figure 10). The null hypothesis was accepted. Potential explanations for these findings include the high prevalence of the slowly metabolizing variant of the aldehyde dehydrogenase gene in Asian populations, which is associated with elevated blood acetaldehyde levels after alcohol consumption, and possibly other non-genetic factors [11]. It was observed that out of 110 subjects, 58.18% have alcoholic habits and the rest drink wine, and beer, and none among the subjects with alcohol dependence, 36.26% are male. Regular habits with 15 units-21 units per week of alcoholism are 48.33% among 182 subjects. CRC of the right colon was found to be 23.33% in 87 subjects. According to previous studies, a positive correlation between alcoholism and tumor location has been reported. But in this study, there was a correlation only with right and left colon cancers and not with others. The alcohol consumption and tumor location were correlated according to the number of units consumed per week. Among the population, more subjects are at (15.21 units consumed) right colon CRC. There was a significant correlation between units of alcohol consumption and tumor location only at the right colon and at the left colon. The null hypothesis was rejected and the alternative was conserved.
Among the dietary characteristics, the Western diet stands out for being rich in fat, animal protein, and calories, as well as low in fiber (fruits, vegetables, and cereals). Red meat, processed meat, and refined carbohydrates contribute to a higher risk. On the other hand, protective substances include calcium, vitamin D, folates, selenium, vitamins, and antioxidants. These are the main factors associated with CRC, although other factors can also influence its development. In addition to higher fiber intake associated with lower meat intake, consumption of fruits and vegetables may reduce the incidence of CRC concerning their content of specific micronutrients such as vitamins and polyphenols.
The carcinogenic effects of red and processed meat are mainly related to the presence of growth-promoting dietary components such as heme and arginine, enhanced by a mutagenic intestinal environment and intestinal inflammatory response. It has been recommended to limit red meat intake to less than three portions per week, equivalent to 350 g-500 g (12 oz-18 oz) of cooked weight. Processed meats, rather than smoked meats and foods containing nitrites should be avoided, as no level of intake can be reliably associated with a lack of risk [12].
The present study showed that the incidence of CRC was 39.91% with consumption of red set and 35.16% with previous habit. The incidence of right-sided carcinoma was observed more in both red meat and processed meat as shown in Table 1. The European Prospective Investigation into Cancer and Nutrition (EPIC) provided strong evidence for this association in more than 500,000 individuals, as regular meat eaters had a 20% higher risk of developing CRC compared to non-consumers or occasional eaters [13]. Similarly, the Norwegian Women and Cancer Cohort (NOWAC), including 88,000 women, concluded that consumption of more than 60 g of processed meat per day doubled the risk of CRC compared to less than 15 g. Other cohorts reported that a daily intake of 100 g of fresh red meat determined a 17% increased risk of CRC, while 50 g of processed red meat increased the risk by 18% [12].
Table 1: Correlation of parameters using Pearson r correlation
| Characteristic | Values | Male | Female | - | - |
|---|---|---|---|---|---|
| Age Vs Gender | *p-value | 0.0001*** | 0.0001*** | - | - |
| r value | 0.9797 | 0.9791 | - | - | |
| Gender Vs time of diagnosis | *p-value | 0.1493ns | 0.4840ns | - | - |
| r value | 0.9726 | 0.7247 | - | - | |
| Gender Vs BMI | *p-value | 0.0005*** | 0.0018** | - | - |
| r value | 1 | 1 | - | - | |
| Gender Vs Employment | *p-value | 0.4764ns | 0.6384ns | - | - |
| r value | 0.7328 | 0.5379 | - | - | |
| Gender Vs Smoking | *p-value | 0.0165* | 0.2459ns | - | - |
| r value | 0.9835 | -0.7541 | - | - | |
| Gender Vs Alcohol Consumption | *p-value | 0.3243ns | 0.7575ns | - | - |
| r value | 0.6757 | 0.2425 | - | - | |
| Age Vs Year of Registration | 2019-20 | 2020-21 | 2021-22 | - | |
| *p-value | 0.0001**** | 0.0001**** | 0.0001**** | - | |
| r value | 0.9959 | 0.9836 | 0.9973 | - | |
| Values | Smoking Vs Location | ||||
| Right Colon | Left Colon | Rectum | Recto Sigmoid | Hepatic flexure | |
| *p-value | 0.0071** | 0.0507ns | 0.0935ns | 0.0146* | 0.2211ns |
| r value | 0.9929 | 0.9493 | 0.9065 | 0.9854 | 0.7789 |
| - | Smoking Duration Vs Location | ||||
| *p-value | 0.3000ns | 0.1878ns | 0.7913ns | 0.5122ns | 0.0877ns |
| r value | 0.891 | 0.9568 | 0.322 | -0.6934 | 0.9905 |
| - | Smoking Frequency Vs Location | ||||
| *p-value | 0.6269ns | 0.5276ns | 0.3180ns | 0.1942ns | 0.4724ns |
| r value | 0.5531 | 0.6758 | 0.8778 | 0.9538 | 0.737 |
| - | Alcohol Frequency Vs Location | ||||
| *p-value | 0.0143* | 0.0488* | 0.0548ns | 0.4186ns | 0.9305ns |
| r value | 0.9857 | 0.9512 | 0.9452 | 0.5814 | 0.06948 |
| - | Food Habits Vs Location | ||||
| *p-value | 0.0004*** | 0.0292* | 0.0694ns | 0.1517ns | 0.0348* |
| r value | 0.9431 | 0.7583 | 0.6695 | 0.5568 | 0.7426 |
The reason for the occurrence of CRC when consumed as a result of excessive dietary fat stimulates hepatic bile acid synthesis, resulting in increased bile acid leakage through ileal reabsorption by the apical sodium-dependent bile acid transporter or ileal bile acid transporter. As a result of their deconjugation by microbial enzymes, the ratio of primary and secondary bile acids entering the enterohepatic cycle and the lumen of the large intestine changes [14]. The second group consuming a high-fat, low-fiber diet has a much higher incidence of CRC compared to the first group consuming a low-fat, high-fiber diet.
The prevalence of CRC increases inversely with fiber intake, which has led to extensive investigation of the protective role of fiber, especially whole grains, in recent decades. Leafy vegetables, fruits, and legumes are rich sources of fiber and are good nutritional foods to protect against CRC. In this study, 24.18% of subjects consume leafy vegetables, 26.37% of fruits and 25.82% have wheat and pulses as a habit. Low fiber consumption may promote CRC progression. Similarly, the European Prospective Investigation into Cancer and Nutrition (EPIC) study documented a 40% reduction in CRC risk in the highest quintile of fiber intake compared to the lowest [15]. Fermentation of fiber by intestinal microflora leads to the production of Short-Chain Fatty Acids (SCFA), mainly acetate, butyrate, and propionate, in a ratio of 3:1:1. Butyrate, in addition to being the main source of energy in normal colonocytes, has a protective effect on the colonic mucosa. Butyrate has anti-inflammatory properties as it has been reported to decrease plasma pro-inflammatory cytokines and increase regulatory T-lymphocytes in animal models [16].
An observational epidemiological study that grouped a sample of 519,978 adults in 22 urban centers in Europe, showed that an increase in dietary fiber reduced the risk of CRC by 25% [17]. Two meta-analyses combining 13 and 20 case-control studies showed that a high-fiber diet reduced the risk of this cancer. Another meta-analysis of 12 case-control studies was selected by Trock et al. (1990) [18].
Milk and other dairy products are thought to reduce the risk of CRC due to their high calcium content. Calcium is thought to protect against CRC through several biological mechanisms, including reduced cell proliferation and promotion of cell differentiation. Although increased milk consumption may reduce the risk of CRC, the evidence is not conclusive [19]. Among the 182 subjects, 23.63% only have the principle of regularly eating dairy products. This may also be the reason for CRC progression in selected subjects as shown in Figure 11. The association of tea/coffee consumption with CRC was still controversial. The effect of tea/coffee consumption on the development of CRC is not well understood. A percentage of 40.11 was observed for regular tea/coffee consumption in 182 subjects. The association is most influenced by the possibility of right-sided and left-sided CRC.
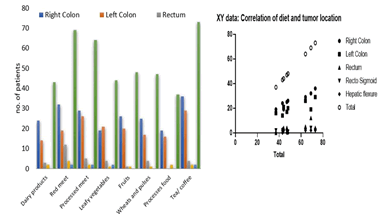
Figure 11: Distribution of study subjects by food habits and tumor location and correlation
Drinking 1 or more cups of iced coffee per week has been linked to an increased risk of rectal cancer. Neither herbal tea nor iced coffee was associated with proximal colon cancer risk. Hot coffee has been associated with a possible increased risk of distal colon cancer. Black tea (with or without milk), green tea, decaffeinated coffee, and milk were not significantly associated with colorectal cancer risk [20]. No significant association was found between coffee and green tea consumption and CRC risk in either men or women. Among women, there was a significant increase in the risk of colon cancer in the group of black coffee drinkers. These partial differences in the effect of coffee consumption on colorectal cancer may be explained by different mechanisms. A previous study found that coffee increased the motility of the colon, particularly the distal colon. Coffee and green tea drinkers are more likely to smoke and consume alcohol. This may be the reason for the increased incidence of CRC in tea/coffee drinkers in this study. Previous studies have reported that smoking has a significant effect modifier on the relationship between tea consumption and CRC risk, coffee consumption increases the risk of rectal cancer in women who have never smoked [21].
Today, there is an increase in the use of ultra-processed foods in our daily lives, but ultra-processed foods contain chemicals that can alter the healthy bacteria in the gut, which can worsen inflammation and lead to an increased risk of colorectal cancer. High consumption of total ultra-processed foods in men and certain subgroups of ultra-processed foods in men and women was associated with an increased risk of colorectal cancer. Among ultra-processed food subgroups, higher consumption of ready-to-eat meat/poultry/seafood and sugar-sweetened beverages in men and ready/heated mixed meals in women was associated with increased risk of colorectal cancer; yogurt and dairy-based desserts were negatively associated with colorectal cancer risk in women. The distribution of subjects by location of tumor and food habits. It was observed that consumption of red meat, processed meat, dairy products, leafy vegetables, fruits, wheat and pulses, processed food, and tea/coffee. Among the selected subjects red meat and tea/coffee consumption was found to be more compared to others. There was a strong correlation between food consumption in the right colon, left colon, and hepatic flexure. The null hypothesis was rejected and the alternative was conserved.
Conclusion
The current study concluded that there was a strong correlation between demographical factors and colorectal cancer and its progression. This was an observational cohort study, which limited the amount of data obtained. Although researchers attempted to contact study subjects individually, data were limited due to irregular patient follow-up over the 3 years. Future prospective studies are needed to better evaluate data and follow-up. It is possible that future research with a larger sample size could be done or it could also be done in some digestive surgery centers.
Acknowledgement
None.
Conflict Of Interest
Authors have no conflict of interest to declare.
References
- K.E. Singh, T.H. Taylor, C.J.G. Pan, M.J. Stamos, J.A. Zell, et al. Colorectal cancer incidence among young adults in California, J Adolesc Young Adult Oncol, 3(2014):176-184.
- R. Schmuck, M. Gerken, E.M. Teegen, I. Krebs, M. Klinkhammer-Schalke, et al. Gender comparison of clinical, histopathological, therapeutic and outcome factors in 185,967 colon cancer patients, Langenbecks Arch Surg, 405(2020):71-80.
- Y. Yang, G. Wang, J. He, S. Ren, F. Wu, et al. Gender differences in colorectal cancer survival: A meta-analysis, Int J Cancer, 141(2017):1942-9.
- N.N. Luan, L. Wu, T.T. Gong, Y.L. Wang, B. Lin, et al. Nonlinear reduction in risk for colorectal cancer by oral contraceptive use: A meta-analysis of epidemiological studies, Cancer Causes Control, 26(2015):65-78.
- G. Luo, Y. Zhang, L. Wang, Y. Huang, Q. Yu, et al. Risk of colorectal cancer with hysterectomy and oophorectomy: A systematic review and meta-analysis, Int J Surg, 34(2016):88-95.
- J. Ferlay, H.R. Shin, F. Bray, D. Forman, C. Mathers, et al. Estimates of worldwide burden of cancer in 2008: GLOBOCAN 2008, Int J Cancer, 127(2010):2893-917.
- N.N. Keum, D.C. Greenwood, D.H. Lee, R. Kim, D. Aune, et al. Adult weight gain and adiposity-related cancers: A dose-response meta-analysis of prospective observational studies, J Natl Cancer Inst, 107(2015):djv088.
- S.C. Larsson, A. Wolk, Obesity and colon and rectal cancer risk: A meta-analysis of prospective studies, Am J Clin Nutr, 86(2007):556-65.
- C.R. Sharpe, J.A. Siemiatycki, B.P. Rachet, The effects of smoking on the risk of colorectal cancer, Dis Colon Rectum, 45(2002):1041-1050.
- V. Fedirko, I. Tramacere, V. Bagnardi, M. Rota, L. Scotti, et al. Alcohol drinking and colorectal cancer risk: An overall and dose-response meta-analysis of published studies, Ann Oncol, 22(2011):1958-1972.
- S.Y. Park, L.R. Wilkens, L.N. Kolonel, K.R. Monroe, C.A. Haiman, et al. Exploring differences in the aspirin-colorectal cancer association by sex and race/ethnicity: The multiethnic cohort study, Cancer Epidemiol Biomarkers Prev, 26(2017):162-169.
- World Cancer Research Fund, Continuous update project report: Diet, nutrition, physical activity and colorectal cancer, AICR, 2018.
- T. Norat, S. Bingham, P. Ferrari, N. Slimani, M. Jenab, et al. Meat, fish, and colorectal cancer risk: The European prospective investigation into cancer and nutrition, J Natl Cancer Inst, 97(2005):906-916.
- Y. Wan, F. Wang, J. Yuan, J. Li, D. Jiang, et al. Effects of dietary fat on gut microbiota and faecal metabolites, and their relationship with cardiometabolic risk factors: A 6-month randomised controlled-feeding trial, Gut, 68(2019):1417-1429.
- A. Sasso, G. Latella, Dietary components that counteract the increased risk of colorectal cancer related to red meat consumption, Int J Food Sci Nutr,69(2018):536-548.
- M. Zhang, Q. Zhou, R.G. Dorfman, X. Huang, T. Fan, et al. Butyrate inhibits interleukin-17 and generates tregs to ameliorate colorectal colitis in rats, BMC Gastroenterol, 16(2016):84.
- S.A. Bingham, N.E. Day, R. Luben, P. Ferrari, N. Slimani, et al. Dietary fibre in food and protection against colorectal cancer in the European Prospective Investigation into Cancer and Nutrition (EPIC): An observational study, BMC Gastroenterol, 361(2003):1496-501.
- B. Trock, E. Lanza, P. Greenwald, Dietary fiber, vegetables, and colon cancer: Critical review and meta-analyses of the epidemiologic evidence, J Natl Cancer Inst, 82(1990):650-61.
- S.A. Lamprecht, M. Lipkin, Chemoprevention of colon cancer by calcium, vitamin D and folate: Molecular mechanisms, Nat Rev Cancer, 3(2003):601-14.
- T.J. Hartman, J.A. Tangrea, P. Pietinen, N. Malila, M. Virtanen, et al. Tea and coffee consumption and risk of colon and rectal cancer in middle-aged Finnish men, Nutr Cancer, 31(1998):41-8.
- I. Kashino, S. Akter, T. Mizoue, N. Sawada, A. Kotemori, et al. Coffee drinking and colorectal cancer and its subsites: A pooled analysis of 8 cohort studies in Japan, Int J Cancer, 143(2018):307-316.
Copyright: © 2023 Shiv Shankar Shav, et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.

